A CAREER IN EMERGENCY MEDICINE = ACTION AND LIFE SAVING PROCEDURES
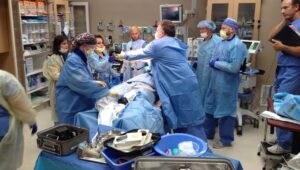
Nearly all medical students have watched emergency room physicians save lives and cure disease on popular television series. They witness the high drama, witty banter, cool procedures, diagnostic coups, and romance. Life (and medicine), though, is usually nothing like the TV show. Does the specialty of emergency medicine really live up to its glamorous image?
Fast-paced and unpredictable, emergency medicine is one of the newest specialties in medicine. It has grown to meet the challenge of 100 million emergency room visits per year. As you know, the ER is always open and easily accessible. Emergency physicians must be prepared for any type of medical problem that arrives at the door, whether by foot, car, ambulance, or helicopter. It is never boring. They take care of a wide cross-section of people of all ages and races, rich and poor, insured and uninsured. These specialists like to work fast and think on their feet while serving on the front lines of medicine.
BUT WHAT IS EMERGENCY MEDICINE?
Emergency medicine involves the immediate care of urgent and life-threatening conditions found in the critically ill and injured. These physicians are really specialists in breadth—their broad-based training encompasses acute problems that span several clinical disciplines. No other specialty can match the astounding variety of patients found within the emergency room. You will see, hear, and smell things that most doctors will not. In just one shift, an emergency physician may care for patients presenting with asthma attacks, atrial fibrillation, gunshot wounds, dislocated shoulders, and even cockroaches stuck in their ears. Every now and then, the EM doctor will discover a zebra, such as a pheochromocytoma (adrenal gland tumor) in a young woman with high blood pressure and headaches.
Emergency medicine became a specialty only about 35 years ago. Until then, most doctors who covered acute, emergent, and traumatic illnesses were actually board certified in other fields, usually internal medicine or surgery.
In smaller hospitals, just about anyone (including psychiatrists) could provide ER coverage for anything from a minor cut to an inflamed appendix. Some of these doctors
left their original specialty to work full time in emergency rooms and grandfathered their way into becoming emergency medicine specialists.
During the 1960s, physicians began to realize that patients would have better clinical outcomes if they received prompt and appropriate care from the moment they entered the hospital. This small group of physicians recognized the need for formal study and training in emergency medicine and subsequently founded the American College of Emergency Physicians in 1968. Over the next 5 years, they worked to establish the first residency program at the University of Cincinnati and lobbied Congress to pass the Emergency Medical Services Act. As a result, emergency medicine began to expand rapidly, using federal funds to develop prehospital emergency systems and to expand emergency departments. In 1979, the American Board of Medical Specialties recognized emergency medicine as an official clinical specialty.
A DAY IN THE LIFE OF THE ER DOC
ER docs provide immediate recognition, evaluation, care, and disposition of a diverse adult and pediatric population. When dealing with acute problems, whether non-urgent or life threatening, their primary role is to stabilize the patient. They evaluate the ABCs (airway, breathing, circulation), take quick histories, perform focused physical examinations, order relevant laboratory and radiology tests, and contact consultants. In the contemporary ED, these specialists must be completely sure that all life-threatening causes of particular symptoms are completely worked up and ruled out. Despite being such a young arm of medical practice, emergency medicine has matured into a rigorous clinical specialty. You will receive formal training to handle just about anything that may walk through that door.
A typical shift in the ED is full of variety, drama, and excitement. As you greet the frequent fliers, who often come for both food and medical care, the chart boxes begin filling up with new patients to be seen. First might be a man clutching his stomach due to abdominal pain caused by pancreatitis. The next patient may be a pregnant woman who presents with vaginal bleeding and cramping abdominal pain—possible signs of an ectopic pregnancy. In this case, you take on the role of gynecologist, conducting a pelvic examination to see if the cervix is open or closed. You may even, depending on your training, take on the role of radiologist in such a case, using a hand-held ultrasound device to determine if the patient has a viable intrauterine pregnancy.
Obviously, the emergency medicine physician has to love juggling dozens of different problems, situations, and treatments while teaching and interacting with patients at the same time. At any time, a code blue (cardiac arrest) or trauma could bring this somewhat orderly environment crashing down. You are generally the first doctor to arrive in the resuscitation room, a place where patients in respiratory distress—with dropping oxygen saturation and pink frothy liquid coming out of their mouths—need immediate endotracheal intubation.
THE MANY SKILLS OF THE ER DOC
For most patients who seek urgent medical care, the EM physician is usually the first doctor on the case. This initial evaluation is both a privilege and a challenge. Patients do not arrive in the emergency room with their medical chart or old records. They may answer your questions poorly.
As such, emergency physicians often have to piece the clinical history together from fragments provided by unresponsive sick patients, family members, EMTs, police officers, and other sources. Being the first person to ask the appropriate questions in a limited amount of time can be frustrating. You must act like a sleuth. You must have the confidence to make fast medical decisions based on limited, incomplete information.
For an emergency medicine doctor, nothing is more satisfying than taking a few bits and pieces of history (and abnormal physical findings), ordering some lab tests, and coming up with a working diagnosis and treatment plan.
While one case is being stabilized, many more are waiting patiently (and often impatiently) for evaluation, treatment, discharge, or admission. The emergency physician constantly juggles many tasks at once, whether acquiring data, making decisions, or performing procedures. Patients, lab results, nurses, chest x-rays, family members, and other physicians all vie simultaneously for your immediate attention. Because you are doing so many things at once, emergency care sometimes requires knee-jerk action, after which additional thinking is necessary. In a short amount of time, you coordinate a wide range of treatment plans, from readjusting an asthma patient’s medications to suturing wounds of another patient who also just received a chest tube. With recent advances in medicine, more and more patients are coming to the emergency room with complex problems, such as unusual drug interactions, or complications from procedures that did not exist before, like organ transplants. Now, emergency medicine specialists find themselves with even more responsibilities to manage at once.
BUT, WHAT ABOUT TRAUMA PATIENTS?
The dramatic, cool procedures that attract medical students to the field of emergency medicine are often performed on trauma patients—people with knife and gunshot wounds, or those who have been critically injured in motor vehicle accidents, drownings, construction accidents, natural disasters, and more. They are quickly transported to trauma centers and met by eager, capable emergency medicine physicians waiting to perform miracles. The idea of saving lives every day excites many medical students and is the strong appeal of this specialty.
A multidisciplinary problem, trauma always involves an entire team of doctors, namely emergency physicians, trauma surgeons, and anesthesiologists. As an EM doctor, do not expect to be the sole individual doing all the work. Typically, the trauma surgeon calls the shots during the resuscitation. After all, the appropriate management of internal injuries due to trauma falls within the realm of surgery. It is important for emergency physicians to recognize the boundaries of their special knowledge and skills. You must learn to appreciate the presence of and guidance by the surgery team with whom you share space.
In saving patients with traumatic injuries, the specific role of the EM doctor depends on the type of trauma and the hospital. First and foremost, all emergency physicians secure the patient’s airway, which can often be surprisingly difficult. For those who thrive on adrenaline-inducing challenges, intubating trauma patients may involve suctioning blood, teeth, or even brain matter out of the way while keeping the patient immobile in a C-collar. Before the surgery team arrives, the emergency doctor continues the rest of the trauma assessment: breathing, circulation, disability, and exposure.
While stabilizing the patient, their role can be quite fluid, depending on the patient’s next outcome. To assess the need for surgery, they might use ultrasound imaging to locate free fluid in the belly of a patient with blunt trauma. Emergency physicians often place central lines and chest tubes. Their most important role, however, is to stabilize the patient until definitive treatment (surgery) arrives. As such, future emergency physicians who want to go at it alone, or who become easily annoyed by orders from surgeons, may find their role in caring for trauma patients much more limited than they anticipated.
WHAT MAKES A GOOD ER DOC?
Likes to work with their hands.
Is adventurous, action-oriented, both a leader and a team player.
Can make logical decision quickly.
Likes variety and the unexpected.
Is capable of juggling many tasks at once.
WHAT IS RESIDENCY TRAINING LIKE?
Residency in emergency medicine requires either 3 or 4 years of postgraduate training. Unlike other specialties, there are actually 3 types of EM residency programs. The majority are 3-year programs that begin immediately after medical school.
During residency, the length and number of shifts worked per week varies per hospital. Regardless of type of program, EM residents also complete rotations in general medicine, critical care, anesthesiology, cardiology, and obstetrics and gynecology. The bulk of their training consists of monthly rotations in adult and pediatric emergency medicine, trauma, toxicology, emergency medical services, and aeronautical medicine. Many programs require a research project.
WHY MIGHT EM BE RIGHT FOR YOU?
Medical students who would thrive on a career in emergency medicine typically like the wide spectrum of clinical challenges and the multidisciplinary approach. As the only specialty in which doctors are required by law to treat all patients seeking care, whether or not they have insurance, emergency medicine can be very challenging. These heroes juggle what seems like a thousand tasks at once, constantly readjusting moment-by- moment plans as events unfold. They also have the challenge of interacting with a dizzyingly varied group of people while caring for their patients, which sometimes involves fighting with the medical staff to make things happen. So, an EM doctor must meet the challenge of being a diplomat and team player. Emergency physicians also thrive on the intellectual challenges. They must be astute clinicians with a solid knowledge of nearly every single organ system and ailment. They really are the only contemporary practitioners who are skilled in the truly broadest range of medicine.
AND HOW MUCH ARE THEY GOING TO PAY ME TO LIVE THE ADVENTUROUS LIFE OF AN ER DOC?
According to the 2020 Medscape Physician Salary Survey, the average salary in the United States for an emergency medicine physician is $357,000 per year. Male emergency medicine physicians make on average $371,000 per year, while female emergency medicine physicians make on average $318,000 per year.
WANT TO BECOME AN ER DOC?
Among medical students, surgery is often times considered the Holy Grail of specialties. Perhaps it is the idea that surgeons solve problems quickly with the flash of the scalpel, and thus have some amount of bon vivant cache in the medical community. Or maybe it’s because then are paid so well for their efforts. Regardless, it is a much sought-after residency program.
But before you can become an emergency room physician, you need to graduate from medical school. And if you are going to pursue emergency medicine, you need a good school behind you. That’s where UHSA comes in. We have been creating amazing doctors since 1982, meaning we know how to help you live your dream.
For those of you have graduated from university and have the premedical requirements, our direct-entry MD program is for you.
If you are still missing some premedical courses, are a recent high school graduate with your eyes set on the prize of becoming a doctor as quickly as possible, then our accelerated premedical program is right for you.
We also offer an innovative joint MD/MPH program that will allow you to graduate with both your medical degree and the much-respected masters of public health. This will enhance your career prospects, as well as prepare you for careers in areas like preventative medicine and international health.
Let us help turn your dream into reality. Contact our Admissions Team today to learn how you can join the UHSA family!

